UI Benefit Accuracy Measurement Report for CY 2006
The Benefit Accuracy Measurement (BAM) program is designed to determine the accuracy of paid and denied claims in three major Unemployment Insurance (UI) programs: State UI, Unemployment Compensation for Federal Employees (UCFE), and Unemployment Compensation for Ex-Servicemembers (UCX). State Workforce Agencies (SWAs) select weekly random samples of UI payments and denied claims. BAM investigators audit these paid and denied claims to determine whether the claimant was properly paid or denied eligibility. The results of the BAM statistical samples are used to estimate accuracy rates for the populations of paid and denied claims. In addition, BAM is a diagnostic tool for Federal and State Workforce Agency (SWA) staff to use in identifying systemic errors and their causes and in correcting and tracking solutions to these problems.
The Improper Payments Information Act (IPIA) of 2002 (Pub. L. No. 107-300) requires agencies to examine the risk of erroneous payments in all programs and activities they administer. An improper payment includes any payment that was made to an ineligible recipient, duplicate payments, and payments that are for the incorrect amount -- both overpayments and underpayments, including inappropriate denials of payment or service. Agencies are required to review all programs and activities they administer and identify those that may be susceptible to significant erroneous payments. The Office of Management and Budget (OMB) has defined "significant erroneous payments" as annual erroneous payments exceeding both 2.5 percent of program payments and $10 million. UI meets both of these criteria. The Department of Labor (DOL) reports to OMB the Annual Report and Operational Overpayment rates, as well as the underpayment rate and improper denial rates, as part of its IPIA report. It is extremely important that BAM accurately measures the level of improper payments so that performance against the targets can be properly evaluated.
Readers are strongly cautioned that it may be misleading to compare one state's payment accuracy rates with another state's rates. No two states' written laws, regulations, and policies specifying eligibility conditions are identical, and differences in these conditions influence the potential for error. States have developed many different ways to determine monetary entitlement to UI. Additionally, nonmonetary requirements are, in large part, based on how a state interprets its law. Two states may have identical laws, but may interpret them quite differently. States with stringent or complex provisions tend to have higher improper payment rates than those with simpler, more straightforward provisions.
UI benefit payments included in BAM in calendar year (CY) 2006 decreased to nearly $30.2 billion, compared with $31.3 billion in CY 2005. CY 2006 BAM paid claims results are based on the 24,396 sample cases completed by April 30, 2007. This represents a completion rate of 99.98 percent. BAM auditors completed claimant interviews for 89 percent of the cases. The remaining audits were completed based on information obtained from agency records, the claimants' former employers, and third-party sources, such as labor unions and private employment agencies.
No single measure can reflect all aspects of UI benefit payment integrity. DOL uses six analytical measures to assess payment accuracy and estimate the risk of erroneous denial of benefits.
BAM Operational Rate (5.93%) The BAM operational overpayment rate includes those overpayments that the states are reasonably expected to detect and establish for recovery -- fraud and nonfraud recoverable overpayments, excluding work search, employment service (ES) registration, base period wage issues and miscellaneous causes, such as benefits paid during a period of disqualification, redeterminations, and back pay awards. Nationally, BAM estimates the operational rate dollars overpaid equals $1.796 billion.
BAM Annual Report Rate (9.99%) - The Annual Report rate includes fraud, nonfraud recoverable overpayments, nonfraud nonrecoverable overpayments, official action taken to reduce future benefits, and payments that are technically proper due to finality or other rules. The rate excludes payments determined to be "technically" proper due to law/rules requiring formal warnings for unacceptable work search efforts. All causes and responsible parties are included in this rate. Nationally, BAM estimates that $3.021 billion in benefit payments were overpaid.
Agency Responsibility (2.93%) - This rate includes overpayments for which the state agency was either solely responsible or shared responsibility with claimants, employers, or third parties, such as labor unions or private employment referral agencies. The rate includes fraud, nonfraud recoverable overpayments, nonfraud nonrecoverable overpayments, official action taken to reduce future benefits, and payments that are technically proper due to finality or other rules. Nationally, BAM estimates SWAs had contributory responsibility for $886.8 million in benefits overpayments.
Fraud (2.72%) The definition of unemployment compensation fraud varies from state to state. The rate includes all causes and responsible parties. Nationally, BAM estimates that $820.9 million in benefit payments were fraudulently claimed.
Underpayment Rate (0.67%) As a percentage of UI benefits paid, BAM estimates the underpayment rate was 0.67 percent or $202.1 million.
For a detailed listing of these rates for each state, click on the following link (note: the spreadsheet may have several pages): Integrity Rates - CY 2006 - all states.xls.
Improper Denial Rates BAM estimates the adjusted improper denial rates to be 10.52% for monetary denials, 5.90% for separation denials, and 9.38% for nonseparation denials.
BAM captures 110 data elements for each sampled payment or denial and DOL uses these elements to produce the various integrity rates listed. Data for eight of these elements are completed only for erroneous payments or denials. The following chart summarizes four paid claim accuracy (PCA) rates, which are used for calculating overpayment estimates.

Each integrity rate represents a different view of the BAM data set. The BAM data construct provides multiple perspectives and payment errors may be included or excluded for a specific rate (See Methodology and Program Description Integrity Rate definitions).
The BAM operational rate is a component of the performance indicator that measures the detection of recoverable overpayments, which is one of five UI program performance goals that the Employment and Training Administration (ETA) has set as part of its Government Performance and Results Act (GPRA) plan. These goals reflect the UI program's benefit payment, tax, and reemployment facilitation responsibilities. Additional information on ETA goals can be found in the U. S. Department of Labor's Strategic Plan for Fiscal Years 2006-2011 at: http://www.dol.gov/_sec/stratplan/main.htm.
The overpayment detection measure is also a Core Measure for UI Performs, the UI performance management system. The overpayment detection measure covers a three-year period for the UI Performs Core Measure and a one-year period for the GPRA measure. The detection of overpayments measure is the percentage of recoverable, detectable overpayments estimated by BAM that state Benefit Payment Control (BPC) operations establish for recovery.
| Overpayment Detection Measure = | Overpayments Established (BPC)
Estimated Overpayments (BAM Operational Rate) |
X 100 |
The operational rate represents that portion of total overpayments that state BPC operations should be able to detect and establish for recovery. The operational rate was defined following an extensive analysis of BAM overpayment data. Overpayment Detection Measure data and individual state results can be found at the following links:
GPRA Measure- http://www.workforcesecurity.doleta.gov/unemploy/gpra.asp
Core Measure - http://www.workforcesecurity.doleta.gov/unemploy/3yr_overpay.asp
The following charts show the cause components of the operational rate and the types of overpayments excluded from the operational rate.
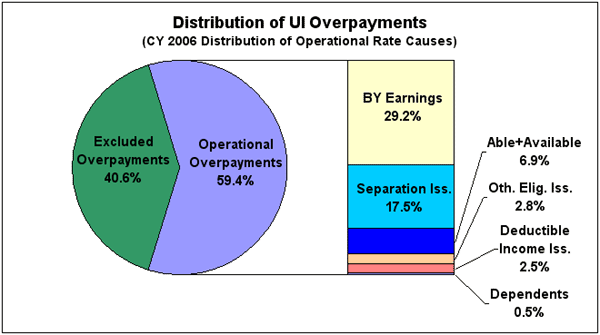
Operational Overpayments
Overpayments included in the operational rate constitute over half of all UI benefit dollars overpaid in CY 2006. More than half of the operational overpayments involve unreported or misreported benefit year earnings. Separation issues account for approximately one-third of the operational overpayments, followed by issues related to the claimant's ability to work and availability for work (A & A). The "Other Eligibility" category includes refusal of suitable work, self-employment, alien status, identity theft, and reporting issues (failure to appear as requested by the state agency to provide information related to the UI claim).
For a detailed listing of these rates for each state, click on the following link (note: the spreadsheet may have
several pages):
Operational Overpayment by cause - all states.xls
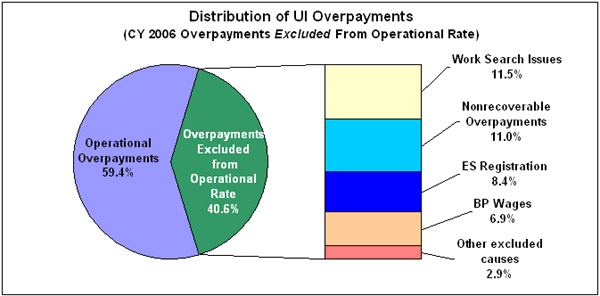
Overpayments Excluded from the Operational Rate
Several overpayment causes are excluded from the operational rate because either 1) state agencies are unlikely to detect these overpayments through the methods commonly employed by BPC (for example, crossmatches of UI claimant Social Security Numbers with wage record and New Hire Directory data, appeals reversals, and tips or leads); or 2) the cost of pursuing these overpayment errors exceeds the amount of benefits that can be recovered. Work search issues (11.5 percent of all overpayments), Employment Service registration issues (8.4 percent), and base period wage issues (6.9 percent) constitute the majority of the excluded causes.
After the exclusions by cause, the residual 11 percent of UI overpayments are excluded because they are unrecoverable, because either 1) the time that has elapsed between the overpayment and its detection exceeds the period established in state law in which an erroneous payment can be recovered (finality rule); or 2) responsibility for the improper payment error rests with the agency, employer, or third party, not the claimant. Most of these nonrecoverable overpayments are separation or continued eligibility issues, such as the requirement that the claimant is able and available for work.
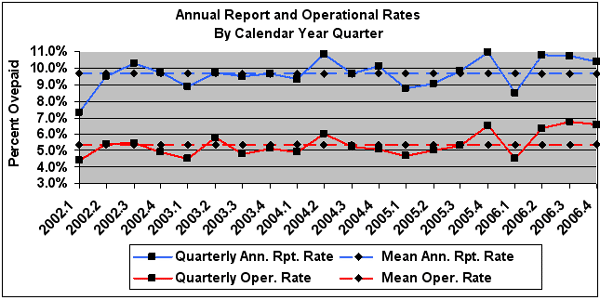
The following chart displays the annual report and operational overpayment rates by calendar quarter. For the period CY 2002 to CY 2006, the average annual report rate was 9.66 percent, and the average operational rate was 5.36 percent.
The chart displays the contrast between these two rates and the impact of excluding the payment errors that are considered "not detectable by normal means" or are cost prohibitive to establish and recover.
For a detailed listing of these rates for each state, click on the following link (note: the spreadsheet may have
several pages):
CY 2005-CY2006 Integrity Rate changes.xls
The distribution of the causes of UI overpayments varies considerably among the four integrity rates. The elements included or excluded from the various rates influences this distribution (See Methodology and Program Description Integrity Rate definitions).
Unreported or misreported benefit year earnings are the leading cause of UI overpayments. They account for over 54 percent of UI fraud overpayments, just under half (49 percent) of the overpayments defined by the operational rate, and nearly 30 percent of the overpayments included in the Annual Report rate, but only 6 percent of the amount overpaid for which the agency had full or partial responsibility.
Separation issues are the second leading cause of UI overpayments. They account for 29 percent of the fraud and operational overpayments, and 26 percent of the Annual Report rate. Separation issues are the leading cause of overpayments for which the agency had full or partial responsibility, accounting for about two-fifths of the amount overpaid.
By definition, work search and ES registration issues are excluded from the operational rate, and account for very small proportions of fraud overpayments. However, ES registration issues account for nearly one-quarter of the amount overpaid for which the agency had full or partial responsibility, and 8.4 percent of the amount overpaid included in the Annual Report rate. Work search issues are a significant cause for the broadest measure of overpayments, the Annual Report rate (12 percent), but are not a significant cause of either fraud overpayments (3 percent) or overpayments for which the agency had full or partial responsibility (5 percent).
| Overpayment Cause By Integrity Rate Percent of the Estimated Dollars Overpaid |
||||
|---|---|---|---|---|
| Cause | Annual | Operational | Fraud | Agency |
| Benefit Year Earnings | 29.6% | 49.2% | 54.5% | 5.7% |
| Separation Issues | 25.7% | 29.4% | 28.8% | 38.3% |
| Work Search Issues | 12.0% | N/A | 2.7% | 4.7% |
| E.S. Registration | 8.4% | N/A | 1.5% | 24.1% |
| Able + Available | 7.2% | 11.5% | 5.9% | 4.7% |
| Base Period Wage Issues | 6.9% | N/A | 1.0% | 6.1% |
| Other Issues | 3.6% | N/A | 1.3% | 7.2% |
| Other Eligibility Issues | 3.4% | 4.7% | 3.2% | 5.9% |
| Deductable Income | 2.6% | 4.2% | 1.2% | 3.3% |
| Dependents | 0.5% | 0.9% | 0.0% | 0.0% |
| Total $ Overpaid - Rate | $3,020,729,192 | $1,796,389,469 | $820,946,831 | $886,813,645 |
Able and available (A&A) issues account for 11.5 percent of the amount overpaid included in the operational rate, 7.2 percent of the amount overpaid included in the Annual Report rate, 5 percent of the fraud overpayments, and only 2 percent of the agency responsibility rate.
For a detailed listing of these rates for each state, click on the following link (note: the spreadsheet may have several pages):
Annual Overpayment by cause - all states.xls,
Operational Overpayment by cause - all states.xls,
Fraud Overpayment by cause - all states.xls,
Agency Responsible Overpayment by cause - all states.xls
BAM identifies the party or parties responsible for all payment errors. As with cause, the distribution of overpayment responsibility varies considerably by integrity rate.
Claimants alone were responsible for 57 percent of the dollars overpaid included in the Annual Report rate. Errors resulting in overpayments that were attributed exclusively to the state agency accounted for 13 percent of the amount overpaid. The claimant and agency were jointly responsible for an additional 9 percent of the dollars that were overpaid.
Claimants alone were responsible for 74 percent of the amount overpaid included in the operational rate. The claimant and agency were jointly responsible for 7 percent of the UI benefits overpaid under the operational rate definition, and the claimant and employer were jointly responsible for an additional 9 percent of the operational rate overpayments.
 * Less than 2 percent of the overpayments were classified as this responsibility.
* Less than 2 percent of the overpayments were classified as this responsibility.
Claimants alone were responsible for 80 percent of the fraud overpayments. Claimants along with employers or agencies were responsible for nearly all of the remainder.
The agency rate is defined by responsible party. The agency was solely responsible for nearly half of the amount overpaid included in this rate. Agencies shared responsibility with claimants, employers, or third parties for the remainder.
For a detailed listing of these rates for each state, click on the following link (note: the spreadsheet may have
several pages):
Integrity Rates by Responsibility - all states.xls
Annual Report Rate Cause and Responsibility - US Total.xls
In the case of payment errors, BAM identifies the action that the SWA took prior to the sample's selection. Prior agency action provides additional details on improper payment responsibility and helps prioritize ways to prevent, reduce, or detect overpayments. At the time the SWA made payment, BAM found most overpayments were not detectable through normal agency procedures. For example, without special actions 78 percent of the operational rate's $1.796 billion overpaid was not detectable.
However, 22 percent of the operational overpayments that BAM found were determined detectable at the time the payment was made. BAM found that at the time sample was selected the agency had resolved or was in the process of resolving just under 7 percent, e.g. separation overpayments, and identified an additional 2 percent of benefit year earnings overpayments through crossmatch with new hire or wage records investigation. For the remainder (12.8 percent or $229.9 million) of the operational dollars overpaid, the agency had sufficient information to identify the overpayment issue but did not resolve the issue, identified the overpayment issue but took the incorrect action, or did not follow the prescribed procedures thereby precluding the SWA's ability to detect the error.
Eighty-six percent of the overpayments determined to be due to fraud were not detectable through normal agency procedures at the time the payment was made. Again, BAM found that special agency actions (e.g. crossmatching with the National Directory of New Hires or taking additional steps to secure employer information) were required to prevent or detect these overpayments. The remaining fraud overpayments were distributed among the other prior agency action categories similar to the operational overpayments.
For overpayments included in the Annual Report rate, a little over two-thirds of the amount of UI benefits that were overpaid were not detectable through normal agency procedures. The agency had sufficient information but did not resolve the issue for 10 percent of the amount overpaid or the agency identified the overpayment issue but took the incorrect action (8 percent). At the time BAM selected the sample, the agency had resolved or was in the process of resolving improper payments constituting 5 percent of the amount overpaid. Finally, for 7 percent of the annual rate dollars overpaid, the agency failed to follow its own procedures.
 *Less than three percent of total dollars overpaid were identified with this prior agency action.
*Less than three percent of total dollars overpaid were identified with this prior agency action.
BAM determined states were responsible (Agency rate) for $886.8 million because they had full or partial responsibility for the overpayment. Of these, the agency had sufficient information to identify the overpayment issue but did not resolve the issue for 34 percent of the amount overpaid; took the incorrect action for 29 percent, and did not follow procedures for 27 percent of the amount overpaid. The remaining overpayments for which the agency had full or partial responsibility were either not detectable through normal procedures at the time the payment was made or the agency had resolved or was in the process of resolving improper payments.
For a detailed listing of these rates for each state, click on the following link (note: the spreadsheet may have
several pages):
Prior agency action for all integrity rates
In the case of payment errors, BAM identifies the action that the employer took before the payment was selected for the BAM sample. Prior employer action provides additional details on improper payment responsibility and helps prioritize ways to prevent, reduce, or detect overpayments. Without special agency actions, BAM considers about two-thirds of overpayments included in the annual report rate to be undetectable by the agencies during their usual payment administration processes, and thus prohibitively expensive for the agency to prevent. Even higher percentages of the overpayments included in the operational rate and fraud overpayments are not detectable without additional procedures. However, BAM detects the majority of its payment errors through the verification of claim information with employers.
Although claimants provide most of the information that agencies use in determining eligibility for UI benefits, agencies also require critical information provided by employers. They provide wage information to the states, which is used to calculate the claimants' weekly benefit payments; respond to notices of new initial and additional claims by providing information on the reason for the claimant's separation; submit notices of new hire, which agencies use to detect claims filed by individuals who have returned to work; and provide detailed information that may corroborate or contradict claimant provided information on issues that affect eligibility, such as availability for work, work search, and job refusal.
BAM data show that prior employer action is a critical factor in the agency's ability to prevent or detect many overpayments. BAM records the following employer actions:
- Employer provided adequate information to SWA in a timely manner for determination.
- Employer provided adequate information after due date for determination.
- Employer provided inadequate/incorrect information in a timely manner for determination.
- Employer provided inadequate/incorrect information after due date for determination.
- Employer did not respond to request for information.
- Employer, as an interested party, was not requested by agency to provide information for determination.
- Not an employer related issue.
Because the state agency uses employer provided information in its eligibility determination process, the accuracy and timeliness of this information affect whether benefits were properly paid. For each payment error, BAM assigns a code to indicate action(s) taken by the employer affecting the Key Week issue as of the date that the sample was selected. Within this coding framework, BAM estimates that employers may contribute to 24.1 percent of the annual report rate dollars overpaid, 18.5 percent of the operational rate dollars overpaid, 17.9 percent to the fraud rate dollars overpaid, and 23.6 percent to the agency responsible rate dollars overpaid.
| Prior Employer Action for Payment Errors | Annual Rate Estimated $ Overpaid | Operational Rate Estimated $ Overpaid | Fraud Rate Estimated $ Overpaid | Agency Responsible Estimated $ Overpaid |
|---|---|---|---|---|
| Not An Employer Issue | $1,486,851,646 | $818,591,715 | $356,248,136 | $372,955,648 |
| Adequate & Timely | $420,229,554 | $291,991,943 | $109,375,908 | $249,814,493 |
| Agency Did Not Request | $385,106,671 | $354,404,269 | $207,981,975 | $54,591,793 |
| Employer Did Not Respond | $322,980,968 | $182,045,922 | $113,610,943 | $93,940,751 |
| Emp. Provided Inadequate | $288,246,466 | $77,700,769 | $6,578,491 | $76,613,787 |
| Emp. Response Not Timely | $92,778,107 | $60,709,372 | $24,265,106 | $27,758,075 |
| Emp. Inadequate & Untimely | $24,535,780 | $10,945,479 | $2,886,272 | $11,139,098 |
| Total Rate Dollars Overpaid | $3,020,729,192 | $1,796,389,469 | $820,946,831 | $886,813,645 |
| Total $ Employer action which contribute to Overpayments | $728,541,321 | $331,401,542 | $147,340,812 | $209,451,711 |
The highlighted sections show estimated overpayments where a different employer action in response to a claim may have produced a different outcome. In other words, overpayments may have been prevented or reduced.
One element stands out in Agency Responsible error rates. For 6.6 percent of the total dollars overpaid or approximately $54.6 million, BAM found that the SWAs did not request information from employers who were an interested party to a determination.
For a detailed listing of these rates for each state, click on the following link (note: the spreadsheet may have
several pages):
Prior Employer Action for all integrity rates -
all states.xls
BAM records the point in its audit process at which it first detects a payment error. Within this framework, it is important to note that the audit process differs substantially from normal UI operations in terms of cost, time, and effort. BAM exhausts all avenues in obtaining information while UI operations make reasonable attempts. BAM detects most payment errors by verifying base period wages, benefit year earnings, and separation information with employers. The data shows taking additional steps to secure employer information or to conduct more in-depth claimant interviews may influence overpayment amounts.

For a detailed listing of these rates for each state, click on the following link (note: the spreadsheet may have
several pages):
Operational Overpaid By Point of Detection and Cause.xls
Point of Detection - all states.xls
For each paid UI week investigated, referred to as the Key Week (KW), BAM records whether the payment was proper or improper and, if improper, the type of erroneous payment. BAM findings of must be consistent with official rules and written policies of the SWA, therefore payment errors are coded accordingly. DOL uses these KW action codes to develop the payment integrity rates discussed throughout this analysis. These integrity rates are defined in "Methodology and Program Description".
Key week action overpayment rates highlight differences in state laws. For example, state laws on work search requirements and finality provisions differ significantly. States may also differ in the way they interpret and apply seemingly identical work search and other UI eligibility requirements. Because state laws vary, state-level data are displayed with warnings not to compare individual state integrity rates. SWAs and state legislators may use key week action error overpayment rates in setting policy priorities or in identifying procedural constraints.
The CY 2006 data are displayed in the following chart.

For a detailed listing of these rates for each state, click on the following link (note: the spreadsheet may have
several pages):
Key week action overpayments.xls
Underpayment Rate
IPIA requires estimates of underpayment rates. BAM estimates that $202 million was underpaid in CY 2006, compared with $206 million in CY 2005. As a percentage of UI benefits paid, the CY 2006 national underpayment rate of 0.67 percent is essentially unchanged from CY 2005 rate of 0.66 percent. State underpayments ranged from 0.06 percent in Maryland to 2.59 percent in Puerto Rico.
Errors in reporting or recording base period wages accounted for over 70 percent of the amount underpaid and represented 0.5 percent of the amount of UI benefits paid. On a quarterly basis, Employers report employee wages to SWAs. States use these wages to establish a claimant's base period, which in turn is used in the calculation of weekly benefit amounts and maximum benefit amounts (See Base Period Wages Report - CY 2006.xls for individual state findings).
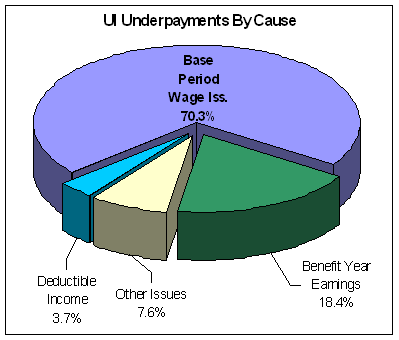
Errors in reporting or recording benefit year earnings were the second leading cause of underpayments – 18.4 percent of all underpayments and 0.12 percent of UI benefits paid. Generally, claimants can work and earn wages while collecting UI benefits as long as they report their earnings. However, weekly UI payments may be adjusted based on claimant reported earnings. For many of these underpayments, the claimant may have over reported their weekly earnings and because of this error, BAM found that UI benefit amount paid was too small.

Employers alone were responsible for almost 40 percent of amount underpaid, which represented 0.27 percent of the amount of UI benefits paid. Claimants alone were responsible for an additional 25 percent of the amount underpaid, which represented 0.17 percent of the amount of UI benefits paid. Because State Workforce Agencies often send out confirmations to the claimant and base period employers at the time of monetary determination, responsibility for these types of underpayments are highly distributed.
The underpayments estimated from BAM paid claims samples represent underpayments only for those claimants eligible for unemployment compensation (UC). Underpayments also result when claims for UC are erroneously denied. Each week, BAM units in the State Workforce Agencies select samples of denied UC claims from three populations, defined by the type of issue on which the denial was based -- monetary, separation, and nonseparation (continued claim filing eligibility).
Denied Claims Accuracy (DCA) Rates
IPIA requires estimates of improper denial rates. DCA measures the accuracy of disqualifying monetary, separation, and non-separation determinations for both intra-and interstate claims. Unlike the investigation of paid claims, in which all prior determinations affecting claimant eligibility for the compensated week are evaluated, the investigation of denied claims is limited to the issue upon which the denial determination is based. DCA investigators verify facts contained in the case file, obtain any missing information, as well as conduct new and original factfinding that may be relevant to the denials determination. The DCA audits record error information in a manner similar to PCA: Dollar Amount of Error, Error Issue Action Code, Error Cause, Error Responsibility, Error Detection Point, Prior Agency Action, Prior Employer Action, DCA Action Appealed, and Prior Claimant Action.
Monetary Denials
State workforce agencies determine the monetary eligibility of claimants when they file a new initial claim or a transitional claim. In CY 2006, SWAs determined that 90 percent of the 11.2 million new initial and transitional claims were monetarily eligible.
BAM estimates that 15.3 percent of the 1.03 million monetary denials were improper. This compares to an improper denial rate of 14.8 percent in CY 2005. The difference of 0.5 percentage points is less than the expected differences in rates due to sampling and therefore is not statistically significant. These UI claims were denied because the agency had initially determined that the claimant had not earned sufficient wages in employment prior to being unemployed or failed to meet other requirements for monetary eligibility, such as sufficient earnings in a minimum number of weeks. The BAM DCA audit identified additional wage credits or an alternate or extended base period for these claimants that had not been included in the original monetary determination or identified other errors in the original determination.
For many of these improper monetary denials, the state agency had identified the additional wages and issued a redetermination establishing eligibility independent of the BAM investigation, or the initial denial was reversed on appeal. When the rate is adjusted for these redeterminations and appeals reversals, the improper denial rate for monetary determinations drops to 10.5 percent, compared with an adjusted improper denial rate of 10.1 percent in CY 2005. The difference of 0.4 percentage points is not statistically significant. Nationally, BAM estimates that 107,955 of the 11.2 million claimants were denied improperly.
Separation Denials
In order to be eligible for unemployment compensation, a claimant must be unemployed due to no fault of their own, discharged for non-disqualifying reasons, or must have voluntarily left employment for a non-disqualifying reason provided in state law, such as workplace harassment, domestic violence, or to relocate with a spouse. Agencies conduct determinations of eligibility when a separation issue has been identified. The agency gathers information from the claimant, employer, and relevant third parties. Based on the findings of fact and the application of state laws, SWAs issue a determination of eligibility.
Separation issues normally are identified when a new initial claim or an additional claim is filed. In CY 2006, there were approximately 10.2 million monetarily eligible new initial claims and approximately 5.9 million additional claims. No separation determination was conducted for nearly three-fourths of these claims, because the reason for separation was lack of work. States completed just over 4 million separation investigations. SWAs found disqualifying circumstances in 1.94 million determinations that resulted in denial of benefits.
In CY 2006, BAM estimated that 8.8 percent of the 1.94 million separation denials issued were improper, compared with 8.1 percent estimated for CY 2005. When redeterminations and appeals reversals are taken into account, the improper denial rate for separations decreases to 5.9 percent, compared with 6.1 percent in CY 2005. Neither difference is statistically significant.
Nonseparation Denials
Nonseparation issues include the claimant's ability to work and availability for work, disqualifying and unreported earnings and income during the benefit year, failure to meet work search requirements, and failure to report as required by the state agency to provide information related to the UI claim or to receive reemployment services. Although nonseparation issues can be detected at various points in the UI claims taking process, these issues generally affect the claimant's eligibility for continued claims of UI.
In CY 2006, Claimants requested payment or "claimed" 131.6 million weeks. Approximately 11 percent of UI weeks claimed were not paid, and no nonseparation determination was conducted. These include weeks for which the claimant did not contest the conclusion of the UI claims taker that the week should not be paid. SWAs made payments for 114.5 million weeks. SWAs completed that 2.9 million nonseparation determinations and concluded that 1.9 million of those investigations should result in denial of benefits.
For these nonseparation denials, BAM estimates an improper denial rate of 12.1 percent and the adjusted improper denials rate of 9.4 percent.
Overpayments and Proper Denials
BAM determined that small percentages of the separation (0.1 percent) and nonseparation (1.6 percent) denials resulted in overpayments. Overpayments can occur if the period of disqualification for UI benefits was less than it should have been, and the claimant received compensation during the period that he or she should have been ineligible for benefits. Overpayments can also occur if the claimant received a partial payment that was too large. A partial payment is a reduction in the claimant's weekly benefit amount and is issued when the claimant has earnings or other deductible income for weeks that he or she claims UI benefits. For some of these compensated weeks, the BAM audit identified additional income that reduced benefits further or in some cases eliminated eligibility for benefits entirely.
For small percentages of all three types of denials, BAM concluded that the claimant was properly denied but the agency committed a procedural error, such as basing the determination on the wrong reason or section of the law or applying incorrect dates to the period of denial. For example, a claimant may have been denied because of a monetary determination that the claimant had earned insufficient wages in the minimum number of weeks required by state law. The BAM audit determined that the claimant did meet the minimum weeks test, but was still ineligible due to insufficient total wage credits earned in the base period. For separation and nonseparation determinations, these errors typically involve citing the wrong issue in the determination (for example, availability versus reporting).
DCA Rates
The following table summarizes the DCA rates described.
| Denial Type | Population of Denials | Sample of Denials | Improper Rate * | Adjusted Proper Rate# | Over Payment | Proper Denial+ |
|---|---|---|---|---|---|---|
| Monetary | 1,026,190 | 7,503 | 15.34% | 10.52% | 0.00% | 0.45% |
| Separation | 1,938,248 | 7,827 | 8.77% | 5.90% | 0.10% | 3.28% |
| Nonseparation | 1,912,432 | 7,819 | 12.11% | 9.38% | 1.64% | 6.15% |
Notes:
In several states, the population from which the BAM DCA samples were selected may not include all of the
determinations that meet the definition for inclusion in the DCA population. This limits the degree to which
inferences about the population can be made from BAM DCA data. States are in the process of resolving these
population issues.
* Improper rate is the percentage of denied claims that BAM DCA concluded were erroneous, whether or not official agency action was taken to issue payment or increase claimant’s WBA, MBA or remaining balance.
# Adjusted improper rate excludes erroneous denials that were corrected by the agency and claims for which eligibility was established on appeal prior to DCA case completion.
+ Properly denied, but BAM identified a procedural error, such as basing the determination on the wrong reason or section of the law or applying an incorrect period of denial.
For a detailed listing of these rates for each state, click on the following link (note: the spreadsheet may have
several pages):
Denied Claims Accuracy Rates -- CY 2006.xls
Agency Action for Improper Denials
Not every improper denial results in the agency issuing a payment to the claimant (or increasing the claimant's weekly benefit amount, maximum benefit amount, or dependents' allowance). Agencies or BAM took action to insure that benefits were paid for just over 79 percent of the improper monetary denials. However, 55 and 60 percent of the claimants improperly denied for separation and nonseparation issues respectively, received benefits. In some cases claimants are ineligible for payment due to other disqualifying issues. In other cases the agency is precluded from taking action because of the time that has elapsed since the denial was issued (finality rules) or by other provisions of the law. BAM records the following agency actions:
- Official Action - Agency took action to issue payment;
- No Payment Due - Claimant was not entitled to payment due to other disqualifying issue or the claimant did not file a claim for the week(s), which were improperly denied;
- Other Improper - No official action could be taken due to finality or other provisions of state law;
- Overpayment - Claimant received payment for weeks of unemployment to which he or she was not entitled;
- Procedural Error - Claimant properly denied, but BAM identified a procedural error on the part of the agency.
The following chart summarizes the type of error by type of denial:
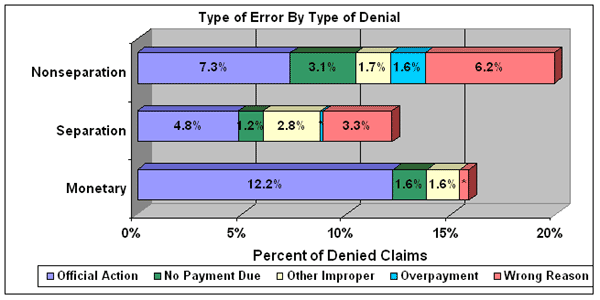
*Less than 1 percent.
For a detailed listing of these rates for each state, click on the following link (note: the spreadsheet may have
several pages):
Improper Denials by Type of Error -- CY 2006.xls
The party responsible for erroneous denials varies by type of denial determination. Employers were solely responsible for almost 28 percent of the erroneous monetary denials due to misreporting or underreporting employees' wages. Claimants were responsible for another 20 percent of the erroneous monetary denials, and agency error accounted for 13 percent of the improper monetary denials.
The state agencies were solely responsible for the 55 percent of the incorrect separation denials and 48 percent of the improper nonseparation denials. Employers and the state agencies were jointly responsible for 12 percent of the erroneous separation denials. Claimants were responsible for over a quarter of the erroneous nonseparation denials.

For a detailed listing of these rates for each state, click on the following link (note: the spreadsheet may have
several pages):
Responsibility for Improper Denials -- CY 2006.xls
Because the state agencies, either solely or jointly with other parties, are responsible for the majority of the erroneous nonmonetary denials and for a significant proportion of the monetary denials, it is instructive to examine agency action prior to the DCA investigation. Agencies had resolved or were in the process of resolving 29 percent of the erroneous monetary denials. However, 43 percent of the improper monetary denials could not be detected through the normal claims taking procedures. Typically, these are claims for which the employer incorrectly reported the wages or the claimant failed to inform the agency that he or she had out-of-state wage credits. Therefore, the agency issued the monetary denial based on the best information available at the time of the initial determination. For improper nonmonetary denials, the agency identified the issue but took the incorrect action for 58 percent of the improper separation determinations and 44 percent of the erroneous nonsepartion determinations.
Although the agency followed its procedures, the issue or information was undetectable for 18 percent of the improper separation determinations and 27 percent of the erroneous nonsepartion determinations. For these claims the agency issued its determination to deny eligibility based on information that, although incomplete, was the best available under normal procedures at the time of its decision.
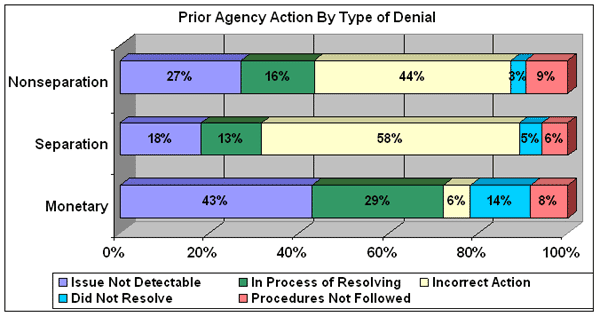
For a detailed listing of these rates for each state, click on the following link (note: the spreadsheet may have
several pages):
Prior Agency Action for Improper Denials -- CY 2006.xls
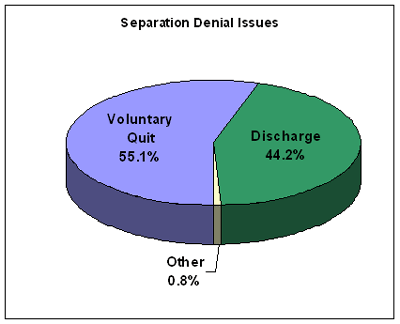
A majority of the separation denials concerned voluntary quits (VQ), while discharges accounted for most of the balance. "Other" includes a small number of labor disputes, military separations, or claimants who were still job attached (partial unemployment).
Claims that were denied for discharge issues were somewhat more likely to be in error than denials issued for VQs. Slightly more than nine percent of discharge denials were improper, compared with 8.3 percent of the VQ denials. Just over 10 percent of the separation denials that were based on "Other" issues were incorrect. The following chart display these separation error rates by type.
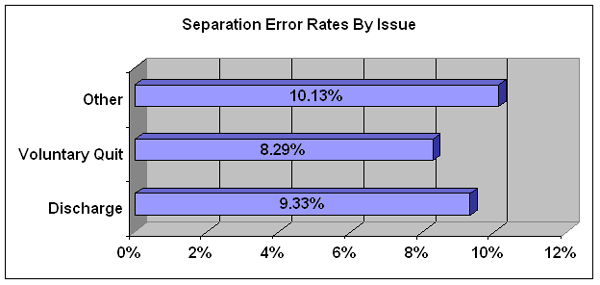
For a detailed listing of these rates for each state, click on the following link (note: the spreadsheet may have
several pages – see the separation page):
Denied Claims Separation Error Rates by State.xls
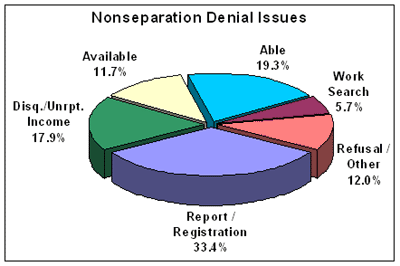
The claimant's failure to report as required by the state agency and provide information related to the UI claim or to receive reemployment services constituted the largest category of nonseparation denials in CY 2006. The remaining nonseparation denials are distributed among several issues, with able and available issues and disqualifying or unreported income issues collectively comprising the majority.
Determinations that denied eligibility because the claimant failed to meet the state's work search requirements had the highest error rate (15.1 percent), although work search issues constitute less than 6 percent on the nonseparation denials. Denials based on the claimant's ability to work had the lowest error rate (5.7 percent). The following table shows improper nonseparation denial error rates by the type of issue.
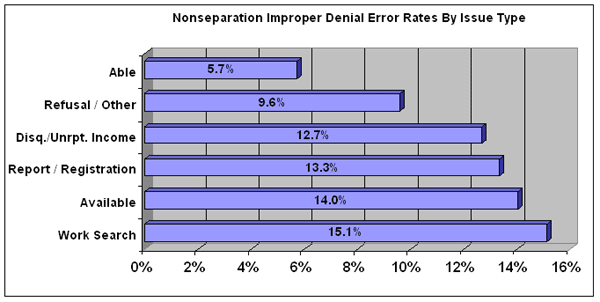
For a detailed listing of these rates for each state, click on the following link (note: the spreadsheet may have
several pages - see the nonseparation page):
Denied Claims Nonseparation Error Rates by State.xls
Links to Additional BAM Paid and Denied Claims Data and BAM Methodology
Integrity Rates*
Integrity Rates - Cause / Responsibility*- Annual Overpayment by cause - all states.xls,
- Operational Overpayment by cause - all states.xls,
- Fraud Overpayment by cause - all states.xls,
- Agency Responsible Overpayment by cause - all states.xls
- Integrity Rates by Responsibility - all states.xls
- Annual Report Rate Cause and Responsibility - US Total.xls
- Prior agency action for all integrity rates
- Prior Employer Action for all integrity rates - all states.xls
- Point of Detection - all states.xls
- Operational Overpaid By Point of Detection and Cause.xls
- Base Period Wages Report by State - CY 2006.xls
- Denied Claims Accuracy Rates -- CY 2006.xls
- Improper Denials by Type of Error -- CY 2006.xls
- Responsibility for Improper Denials -- CY 2006.xls
- Prior Agency Action for Improper Denials -- CY 2006.xls
- Denied Claims Nonseparation Error Rates by State.xls
- Denied Claims Separation Error Rates by State.xls
- BAM Integrity Rate Definitions and Methodology
- BAM State Contacts
- ET 395 Handbook 4th Edition BAM State Operations Guidance
- Electronic Code of Federal Regulations - Quality Control in the Federal State Unemployment Insurance System
- Comparison of State Unemployment Laws
- Significant Provisions of State Unemployment Insurance Laws
- ET 301 Handbook 5th ed - nonmonetary determination guide sheets
*The Excel spreadsheets may have several pages of data.
Prepared by:
U. S. Department of Labor
Employment and Training Administration
Office of Workforce Security
Division of Performance Management
July 2006